I didn’t have the birth I wanted this fifth and final time in labor and delivery, and despite my delectable baby girl, I’m sad about it.
Like her siblings before her, my plan was to bring sweet little baby number 5 into the world using hypnobirthing (which is exactly as improbably magical as it sounds) and lots of time in the tub. I packed my only swimsuit top—a super inappropriate Victoria Secret purple leopard-print push-up number—and some chill Apple Music playlists, as well as a ton of books, travel sizes of my most indulgent shower and beauty products, and some of my favorite sheet masks, imagining a lovely private baby moon in the postpartum ward while my husband wrangled the rest of our kids at home and I basked in the glow of that special endorphin high that you can only achieve after a med-free birth.
Since I wasn’t going to have any meds, my little baby would be alert and ready to nurse like a teeny tank right away. I wouldn’t be numb, so I could take the world’s hottest shower while she slept off birth. I would not go to the hospital until I was at least 5 cm dilated, so my 14 year-old could hold down the fort at home no worries, and my husband could welcome his new daughter and head home, leaving the two of us to cuddle and sleep for a couple of days.
I should mention that I am 42, and because of my age, my midwives recommended lots of extra monitoring at the end of pregnancy because old moms have a higher risk of stillbirth. This risk is so great, in fact, that the standard is to induce moms my age on our due dates and throw in lots of extra monitoring the last 2 weeks of the pregnancy. Starting at 38 weeks, I needed a midwife office visit, an ultrasound, and 2 nonstress tests a week.
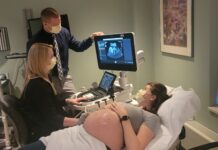
At 38 weeks and 2 days, I had my first of these eleventy billion appointments: an office visit and a nonstress test. My office visit was unremarkable except I gained 2 more pounds to equal 34 total pounds, most of them Oreos. For the NST, I settled into a recliner with 2 monitors on my belly—one to keep track of contractions, the other for the baby’s heart—and a good enough thriller to read. I listened to the baby’s galloping heartbeat and watched the machine spit out strips of paper with a map of my contractions (minimal) and the baby’s cardiac response.
I thought everything was going fine and was looking forward to having 3 more of these relaxing encounters on the books. And then my nurse came in to read the map of contractions and heartbeat produced by the machine. “Uh-oh,” she said.
That uh-oh changed everything. The baby was having late decelerations in her heartbeat when I had mild contractions, and these are the kind of decelerations that happen when the placenta is maybe not getting enough blood. In other words, they are exactly what all of that extra monitoring is for.
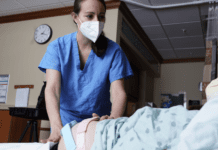
That morning, I had been poolside with my kids. By 4pm, I was in my labor and delivery room with a midwife watching fetal heart tracings on the screen with a frown and talking to my OB about a c-section. By 9pm, I had an IV, a giant bag of fluids, a cervix that was waaaaay in the back and not even a little bit dilated, and a dose of cervidil. I slept off and on while the cervidil did its thing, and I woke up the next morning 1 cm dilated, with a cervix pointing off to the side like the arrow on an I’m With Stupid t-shirt. A few hours with a Foley bulb got me to 3 cm, cervix finally reporting for duty front and center and fully effaced. A full TWENTY FOUR HOURS after I checked in to the hospital, I started on a Pitocin drip. My husband came racing back to the hospital late that night when the baby was tachycardic and it looked once again like we were headed to the OR, but she stabilized; he went home, and my marathon labor continued.
Thanks to the magic of waterproof monitors, I labored in the tub for a few hours, but you guys! Pitocin contractions are no joke, and all the hypnobirth mantras in the world could not stop me from screaming EPIDURAL (I did use the breathing techniques while I had LITERALLY TEN CONTRACTIONS back-to-back while the anesthesiologist worked his magic, though—shout out to the wonderful nurse who let me squeeze her fingers).
By the time my husband came back, more than FORTY HOURS after I was admitted, I was numb and happy, but this relief was short lived. I started feeling immense pelvic pressure; my legs were tingly, and I swore I felt something wet and said a little prayer that it was not my catheter.
“Let’s check you,” the midwife said. “I bet it’s time to push.”
I hadn’t eaten since breakfast two days prior to this moment, and I had barely slept in this same amount of time. I closed my eyes and did a few deep breaths, wondering where I was going to find the strength to push the baby out, when my midwife gasped.
“Your water broke.” she said. “And the baby! She’s right here. Look at all that hair! You’re going to have a baby right now.”
Equal parts shocked and thrilled, I laughed.
“Laugh again,” she said, “And you’ll have a baby.”
So I did. AND WE DID.
Still, it wasn’t the labor I wanted. I checked out of the hospital 24 hours after she was born, spa plans be darned, because I needed to SLEEP. My milk took a hot second to come in, and my baby, all puffed up from liters of IV fluids, lost too much weight and needed me to pump and supplement for a day. I had to wait ages for a postpartum shower because I couldn’t feel my legs. I will never ride the natural birth high again, and my last L&D experience was the most stereotypical slew of interventions I could imagine.
Sure it ended with the perfect baby I am holding while I type this with one hand, but neither one of us was ready for labor that fateful day at the midwife’s office, and I will always long for the gentle L&D experience we never got to have. And you know what? I think that’s ok. You can be grateful it all worked out and be sad to abandon your plan.
Have you had a labor that was different than the one you wanted? How did you deal with the emotions?
















Two kids. Both times it did not go as planned. With the first, I wanted the epidural and HATED. IT. Freaked out because I wanted to get up and walk. Very nearly ended up with a C-section. Epidural wore off during the 2.5 HOURS of pushing. Cord wrapped around his neck twice so no baby-on-chest moment.
With the second, I had to be induced because I was 39 with gestational diabetes. I did NOT want to be induced and did NOT want the epidural but got one after I ripped my husband’s shirt down the front with my bare hands. Nurse was patronizing of 38-year-old, second-time Mom.However, once I got the epidural I actually did feel better, except for the two inch round spot on my upper stomach area that I could feel EVERYTHING in, and she was born easily and placed right on my chest. However, I sprained my diaphragm pushing her and couldn’t breathe right for a week.
They both rock. Worth every second
My first kiddy’s birth was hard and scary (24 hours of labor, c-section because of placenta/heart rate issues). I was physically and emotionally done, so the little setbacks about needing to supplement with formula, etc. felt cataclysmic. When we left my husband said our son’s birth was the best day in his life. It wasn’t for me. But there have been many, many best days of my life with my son since.